How Does Diabetes Affect My Eyes?
What is diabetes?
Diabetes is a very common chronic health condition that affects how the body processes nutrients. Over 37 million people in the US have diabetes – that’s about 1 person in every 10.
Normally, the body breaks down most of the food you eat into sugar (glucose) and releases it into the bloodstream. When blood sugar goes up, it signals the pancreas to release insulin: a hormone that allows blood sugar to be used as an energy source. With diabetes, there is either a lack of production of insulin (Type I), or the body is not able to use what insulin it does make properly (Type II). This means glucose will stay in the bloodstream rather than being processed and sent to your cells for energy.
If diabetes is not properly managed through treatment or lifestyle changes, it can lead to serious health problems including heart disease, nerve damage, higher risk of stroke, and vision loss. Many people with diabetes are still able to live long, healthy lives; but a key aspect of that involves becoming aware of potential health risks and taking steps to avoid them.
How does diabetes affect the eye?
Poorly managed diabetes can lead to frequent episodes of high blood sugar. This can cause problems in two important structures in the eye: the lens, and the retina.
In the short term, episodes of high blood sugar can cause swelling of the lens, which causes blurred vision. This effect is temporary and goes away as sugar levels return to normal.
When there is too much glucose in the bloodstream that the body is unable to use, some of it is deposited into the lens (a structure in the eye that is critical to our vision). Ultimately, this leads to “swelling” of the lens, which can cause episodes of noticeably blurred vision. These episodes can be very inconvenient and decrease the effectiveness of correction such as glasses or contacts.
Cataracts
Cataracts are typically a product of aging and occur when the lens in the eye becomes cloudy over time, leading to blurred vision that is not correctable with glasses or contacts. Diabetes can accelerate the development of cataracts due to buildup of deposits in the lens from episodes of high blood glucose. With adequate diabetic management, however, this risk can be diminished.
Retinopathy
In the long-term, diabetes can affect another crucial structure of the eye: the retina. This inner lining of the back of the eye is what senses light and actually turns it into a message that your brain is able to interpret, letting you see the world around you.
Chronically high blood sugar levels can damage blood vessels in the retina, resulting in leaked fluid and swelling. This condition is called nonproliferative diabetic retinopathy, or NPDR. With proper diabetic management such as medication, dietary changes, or other lifestyle changes, the risk NPDR can be minimized.
However, if the disease gets worse, proliferative diabetic retinopathy (PDR) may develop as new blood vessels to grow on the retina to replace others that have weakened or closed off entirely. PDR may also result in macular edema, which is swelling in an area of the retina called the macula that is responsible for our central vision and helps us read, drive, and see faces. Over time, these conditions can lead to serious and possibly irreversible vision loss.

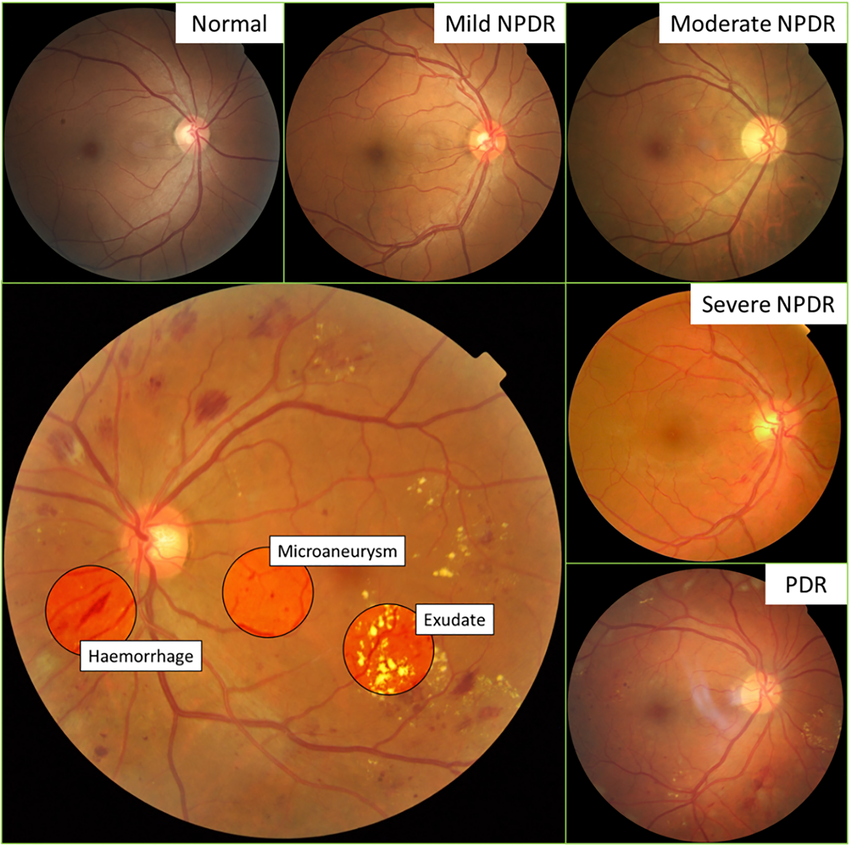
| Examples of the retina of a normal eye, and eyes that have been affected by diabetic retinopathy. |
What can I do to protect my eyes?
Knowledge is power! The first step someone should take after being diagnosed as diabetic is schedule a dilated eye exam, which is typically recommended by the primary care physician upon diagnosis. During a diabetic eye exam the provider will assess the eye for any diabetic damage and provide treatment if necessary. It is critical that the patient is dilated at this exam, which allows the provider to get a full view of the entire retina and look for any signs of retinopathy.

| Your eyes may seem fine, but having a full, dilated eye exam is the only way to know for sure. |
The risk of vision loss from diabetic damage can be minimized by working with your primary care provider to manage your diabetes through diet, exercise, and taking medication as prescribed. Be sure to make regular appointments with an eye care professional to monitor for any early signs of damage.
Sources cited
Centers for Disease Control and Prevention. National Diabetes Statistics Report: Estimates of Diabetes and Its Burden in the United States, 2014. Atlanta, GA: U.S. Department of Health and Human Services; 2014.
Diabetic retinopathy preferred practice pattern guidelines. American Academy of Ophthalmology website. https://www.aao.org/preferred-practice-pattern/diabetic-retinopathy. Updated January 2016.
Tajudin, Nurul & Kipli, Kuryati & Hamdi, Mahmood & Lim, Lik Thai & D.A.A, Mat & Sapawi, Rohana & Sahari, Siti & Lias, Kasumawati & Jali, Suriati K & Hoque, Mohammed. (2022). Deep learning in the grading of diabetic retinopathy: A review. IET Computer Vision. 16. n/a-n/a. 10.1049/cvi2.12116.
